 Visit Elective Africa website Visit Elective Africa website
|


|
|
|
| Elective Africa Monthly Newsletter |
 |
|
How do you tell someone that a person they love is dying? Are there any right words to say? Is there a way to prepare a terminally ill person for it? In this newsletter we share with you some advice from Dr. Nelly Bosire on sharing bad news with patients and their loved ones. The World will commemorate Hypertension Day on 17th May for the 12th time since this day was founded. Find out more on the rising disease burden of hypertension in Kenya and some of the factors fuelling the spread. In our case studies Tanya Raven a recent participant of the Mental Health Nursing Elective summarizes her experience in Mombasa Kenya. Find out on what her highlight for the placement was. Do you have a healthcare topic of interest? Talk to us to guest write for our readers and let us share together. Back to top |
| Sharing the Bad News with Patients by Dr Nelly Bosire |
 |
|
A few years ago, I met a patient who had cancer that could only be treated surgically. She had gone under the knife seven times without respite. I met her when the cancer had reared its ugly head again, but there was no way she could survive another surgery. Despite this information, she adamantly demanded surgery and kept moving from one doctor to the next, hoping to find one who would do something. She chased away the terminal care team whenever they came to see her because she did not want to accept the eventuality of death. We are all going to die, but death feels more real for a person with a chronic terminal illness. Seeing death coming at you like an oncoming train to a person stuck on the railway track is frightening, not just for the patient, but also for their loved ones and caregivers. As the patient suffers, the family and caregivers silently endure deep turmoil. Desperation to stay alive has led patients to traverse the world in search of a cure, yet many patients seeking treatment abroad still end up with the same prognosis. They still die of the disease but what may differ is the experience of the death itself. Wait and See Some seek alternative treatments, such as traditional healers, religious interventions and praying for miracles, which they would never have given second thought to in different circumstances. Different people handle impending death differently but the underlying emotions range from despair, anger, self-doubt, guilt and desperation. A father with young children who is caring for his dying wife will be in agony over losing his loved one and the bleak future of his children growing up without a mother. He may feel like he didn’t try hard enough to keep his wife alive, even when it is glaringly obvious that there isn’t anything anyone could do to change things. The medical team does not fare any better. Doctors, nurses and other healthcare workers are repeatedly traumatised by the death of their patients. Long-term care of a patient, from diagnosis to death, leaves one drained emotionally, yet medics in Kenya have not been sufficiently trained to deal with patients who are on the verge of death. Many feel ill-equipped to tell the patient and his/her family that there is nothing that can be done to avert death. They do not know how to deal with the “do nothing” phase of the patient whose death is unavoidable after all medical interventions have failed. While nobody wants to die, when death is inevitable there should be a way to prepare the patient for it. However, death preparedness is still a relatively new concept in our culture. It requires continued, honest and accurate communication between medical professionals, the patient and his family. This communication must be initiated at the first point of contact. The doctor must explain the diagnosis, its implication, expected course of the disease as per documented evidence, available treatment options (even if they’re not available locally), the expected outcomes of treatment, the possibility of treatment failure and eventual death. This information arms the patient and family with knowledge on what to expect and eliminates the element of surprise. Every new situation is anticipated and mentally prepared for.There is often a danger of doctors promising too much in a bid to reassure the patient, making it difficult to handle negative outcomes when they come. Without candour, the patient and his family, who have just received the bad news, are desperate to hang on every rope thrown at them, however feeble. Quality of Life Then when things take a downward turn, mistrust develops between doctors and their patients, leading to decisions that might be harmful. Palliative care in Kenya is still a neglected entity. Most doctors bring in the palliative care specialists when all curative treatment options have been exhausted. The ideal is that the palliative care team must be involved from the beginning of care for a patient with a chronic disease with possible poor outcomes. This allows the patient to feel comfortable with them and not just to associate them with death. Palliative experts participate fully in improving the patient’s quality of life as he goes through various treatments and their adverse effects. With time, as the end approaches, they are able to take on a bigger role in the patient’s care as aggressive treatments are stopped. Focus on the psychological and spiritual aspect of the patient is as critical as focus on the physical. If a patient can feel death coming and remain calm, acceptance for the family becomes easier. I have seen a hospital employ a cello player who would sit in a corner of the patient’s room, playing soothing music as the family bid their kin farewell. As caregivers, it is our duty to ensure the patient is fully supported to accept death, to help them put their affairs in order and to allow them to move on to the next world with dignity. Adopted from the Healthy Nation 25th April (www.nation.co.ke) Back to top |
| Hypertension the Silent Killer |
 |
|
On 17th May every year, the World celebrates World Hypertension Day which was founded in 2005. The focus of this year is Know your Blood Pressure but there is very little attention given to this condition by the policy makers. In Kenya for example a study conducted by AstraZeneca shows that 15 % of the Kenyan adults suffer from blood pressure. The Rise of blood pressure as a top morbidity contributor mirrors the escalating levels of non-communicable diseases in the developing countries. By 2020 it is projected that non-communicable diseases including, hypertension, will outstrip communicable diseases as the leading cause of death. Demographic changes, increasing urbanisation and lifestyle changes are some of the factors contributing to the increasing burden of NCD. Hypertension in Numbers:
Reasons Behind Rise of Hypertension in Kenya Non-communicable lifestyle diseases such as hypertension have historically been the preserve of the rich in Kenya. But this is changing, primarily due to urbanisation, which has affected the lifestyles of low income earners. In Kenya 22.3% of the population is urban with an urban population growth rate of 4.2% almost double the national population growth rate of 2.4%. Urban population growth and increase in the number of urban inhabitants means that more people now live in slums and informal settlements which further exposes them to more risk factors. Among other factors fueling this spread are:
Possible Complications from Hypertension Here is a list of some of complications that may arise as a result of this condition
To curb the spread and the fatalities arising from hypertension, its important to first realize that majority of the hypertensive subjects in Kenya are undetected and therefore unaware of the risks they face. This is a major impediment to control of hypertension. There is therefore need for greater awareness of hypertension in the general population and health care givers. Greater emphasis also needs to be placed on detection, treatment and control of high blood pressure. Preventive efforts targeting behavioural lifestyle changes, at community level, to curtail these risk factors at population and individual level is also an essence as a strategic move to curb diabetes. Low resources available to adress the rising trends in NCDs among them hypertension is a constant reason for their increasing contribution to mortality and morbidity. The campaign of this year’s world hypertension day is Know your blood Pressure. Do you know yours? Back to top |
| See what clients say about us - Elyssa Metas |
 |
|
My four weeks at Mt.Meru Regional Hospital OBS&GYN Department have been an incredible learning experience.The doctors and staff have been welcoming and willing to teach.The department is extremely busy and there lots of opportunities for hands on including deliveries. Where Elective Africa really shines is with their program Coordinators. Our Coordinator in Arusha has been outstanding. He has gone above and beyond to make our experience here unforgettable. I would recommend EA to any Senior Medical Student looking to do an elective abroad. Elyssa Metas Back to top |
| "My Placement in Five Minutes" Tanya Raven |
 |
|
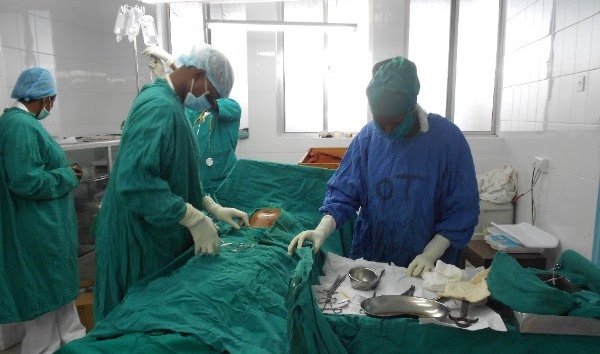
Meet Tanya Raven, a second year Mental Health Nursing Student from The University of Nottingham in England. Period of Placement - 4 Weeks Program - Nursing Elective Placement Hospital - Coast Provincial General Hospital, Mombasa, Kenya What are the main reasons as to why you choose Kenya as your destination of choice? I was looking for a place in Africa to work within the gender based violence. In the course of my search Elective Africa came up and appeared to me as the best opportunity for me and this opportunity packaged in the way I desired was present in Kenya and Mombasa, Kenya to be precise. It was easy for me therefore to choose it as it presented exactly what I wanted. What was your general expectation as you travelled to Kenya, and as you started off your rotation? My choice of Kenya was of course informed by my desire to learn and experience mental health nursing in a different cultural setting. My general expectation was to see how the health system here deal with issues relating to GBV. I also expected to learn more on how the nursing care differs with England. It was also in my expectation to learn about culture and social effects that influence the health and wellbeing of the population and possibly borrow leaf and learn something to take back to England. What are some of the key health concerns in the region you were placed for an elective? If I was to state one, I would definitely agree with the statistics of Kenya, that HIV/ AIDs is a major problem for the health system. There is inadequate accessibility to the health services and the minimal resources making the delivery of care really constrained across the various conditions. What are some of the experiences you had in the hospital of placement, that shaped your rotation/elective? Elective Africa program allowed me flexibility to rotate in other departments aside of my main interest department that was very rewarding. One of the experiences was in the labour ward where I got to see the Caesarean section and how it is conducted. This was both an amazing experience and a tragic experience for me but very educative I must say. With regards to my main area of objective working with the nurse at the gender based centre and listening to her counsel people was definitely amazing and the nurse was friendly and overly inspirational. What would you say in your opinion are the challenges in the delivery of care in the hospital you were placed at? Low resources levels(funding) would be my number one challenge in the GBV center that was evident and also in the labor wards its something that was outrightly observable. The health care professionals have to greatly improvise but some services can only be delivered when the resources are adequately present. Resources shortages is a big challenge. What was your best moment during your placement in Kenya ? At the hospital, seeing people being counselled was amazing but the best of it was the sight of relief in the patients when for example a HIV test came out as negative. Basically the whole experience of a new health system, new ways of care delivery and different culture was all very rewarding. On the Recreational aspect, the excursions organized by the local elective Africa staff, Phares and Benson, were very exciting rewarding and fun. To mention a few, visiting Holla park, seeing Giraffes and getting to hold a crocodile and put it on my head was very amazing. Visiting the south coast beach was also amazing. The comfort and company given to me by the other students from Hong Kong and sharing perspectives with them was actually a very great experience that made my stay great although I had travelled alone. Is it something you would like to have again? Absolutely! This is an experience I would like to have again. Once I qualify I would like to come back and volunteer for a longer period and be able to help. I would definitely choose to come with Elective Africa. Any Parting shot? My advice to anyone thinking of travelling for an elective abroad, Elective Africa is the best you can ask for. Also get to learn a bit of Swahili. I end by saying Kwaheri – goodbye and Asante – Thank you, The top Swahili words I learnt. Learning Swahili was very amazing as well. Back to top |
|
|

 5 2017
5 2017