 Visit Elective Africa website Visit Elective Africa website
|


|
|
|
| Vaccines: The Tugboats of Preventive Health |
|
Welcome to this Month’s Newsletter. Each month has a special favor, a feeling that is unique to its own transitional span of time. June is the symbol of brightness and radiance. This Month our focus is on the challenges Kenya is facing towards its mass Measles-Rubella Vaccination drive that ended recently. This is an important read especially for students who are planing their medical electives abroad so that they can get a glimpse of the healthcare system in the developing world and perhaps do their healthcare internships abroad to gain an invaluable experience in their career. In the second article we focus on drug resistance and how costly it is to treat diseases with antibiotics. Kenya's new nightmare after Malaria is Pneumonia which claims 22,473 lives in Kenya yearly. Sitawa Wafula is a Mental Health Activist who suffered from a Bipolar Disorder. Her condition did not put her down but gave her the limelight to advocate for mentally ill people. Read her inspiring story in our last topical segment and get more insights about this disorder and its impact on peoples lives. Elective Africa has been in business for over fifteen years and has served mainly healthcare students quench for medical internships abroad with superior support services. We are all about service, making a difference and building a global community. Happy New Month!!! Back to top |
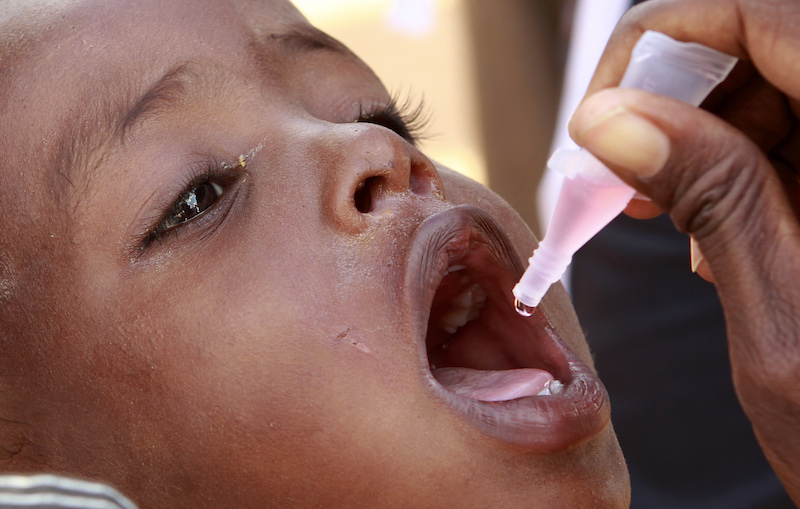
| Measles and Rubella Vaccination Drive |
 |
|
“Childhood Vaccines are one of the great triumphs of modern Medicine. Indeed, parents whose children are vaccinated no longer live to worry about their child’s death or disability from Whooping Cough, Polio, Measles, Diphtheria, Hepatitis or a host of other infections”, Ezekiel Emmanuel. Kenya conducted its first countrywide mass Measles-Rubella Immunization Campaign from 16-23 May 2016 in an effort to prevent 18,000 infant and child deaths. “Vaccines keep children alive and healthy by protecting them against diseases. However, in Kenya vaccine preventable diseases remain a major challenge with an estimated 450,000 children not fully immunized.” said UNICEF in a statement. Children will get Jabs of a new combined Vaccine which offers them double protection against Measles and Rubella which can cause severe birth defects and still birth. According to Heath Principal Secretary Nicholas Muraguri, Rubella also known as German measles can cause deafness, blindness, heart conditions, intellectual impairment and a host of other disabilities. The disease is caused by the genus Rubivirus mostly found in airborne respiratory droplets and it causes congenital anomalies known as congenital rubella syndrome (CSR) a deadly element of Rubella. Rubella symptoms are similar to those of Measles and include red rash, fever, painful joint and muscle spasm, clenched teeth and swollen lymph glands around the ears and the back of the head. Up to 50 per cent of Rubella victims may not show symptoms. The difference between Rubella and Measles is that Rubella is considered to be a milder disease that only lasts around three days; Measles can become a serious illness that lasts several days and can cause other serious permanent complications. A disease surveillance conducted by the Health Ministry in 2014 shows that of the 1,570 suspected Measles cases,557(30 per cent) turned out to be Rubella with over 97 per cent patients being children under 15 years.Girls and women aged between 14 to 49 years received Maternal Neonatal Tetanus Vaccination in 24 high-risk sub counties. A member of the Measles and Rubella technical advisory group, Prof Ruth Nduati said that Kenya required 21.8 million doses of the MR vaccine,23.5 million syringes,Health workers and Volunteers in order to eliminate Measles-Rubella. This is the first time the country conducted a Vaccination Campaign for more than five days, other campaigns have been lasting between three to five days. In the recent past, Vaccination Campaigns have been severely hampered by opposition from Churches and other groups. In 2015, The Kenya Conference of Catholic Bishops and The Kenya Catholic Doctors Association warned Kenyans that the Tetanus Vaccine Campaign undertaken by the Ministry of Health was contaminated with hCG. Findings on samples collected by the Catholic Doctor’s Association expressed concern that the Vaccine Program was being used to conceal a Population Control Campaign in Kenya, especially because the target group were women in child bearing years. UNICEF and WHO were forced to mount huge media campaigns to convince Kenyans that the Tetanus Vaccine was safe and sought to dispel what they termed as misinformation from the Catholic Church. This year the mass Vaccination Campaign for Measles-Rubella in Kirinyaga and Tharaka Nithi Counties started with a hitch as the Catholic Church and parents opposed the Measles Jab. Kirinyaga Health Executive Wambui Miano said 198,546 children aged between nine months and fourteen years needed the Vaccination but the County might not meet the target due to frustration by the church. Measles Vaccine is always present in Health facilities and lack of proper sensitization causes consistent pattern in its partaking. These are medical realities in the developing World that one should be keen to learn and discover about during their elective abroad internships. Good health and good sense are two lives’ greatest blessing. Back to top |
| The Pain of Antibiotics Drug Resistance |
 |
|
The emergence of bacteria resistance against drugs targeting them is raising global concern among Healthcare workers, Governments and Policy makers. According to WHO 2014 report, resistance to respiratory, urinary tract and blood infection antibiotics has emerged posing serious threats to managing pneumonia, malaria, urinary tract infections and chronic illnesses like tuberculosis and HIV. Previously the extent of the problem was thought to be in developing Countries mainly but this is not the case. Increasing patient mobility and more intimate interactions among global citizens allows resistant bugs to now be carried all over the World. A year ago social media was awash with talk of a “super bug” that was transmitted through sexual contact that raised concern in North America. The Centre for Disease Control (CDC) data also hinted the concern. The impact of this problem is not just limited to the global health aspects, but also financial consequences to Health Systems. The global projected cost of the resistance is in hundreds of billions of dollars and has the potential to escalate. Antibiotic resistance means multiple drugs have to be used for treatment of one condition and the duration taken for recovery may be prolonged meaning lengthier hospital stays.On the health angle, common conditions previously salvageable will now progress to severer forms. Several reasons have been given for this emerging phenomenon, among them the non-adherence to drug prescriptions, treatment guidelines, repeated exposure to substandard medicines and poor pharmacovigilance. As measures towards arresting this, the WHO recommends that antibiotics be prescribed only when necessary and if possible for the specific bacteria causing the infection. In many health setups however, the crucial laboratory tests needed to identify the offending bacteria are missing. As a result, many infections are treated on an empirical basis.Looking across our labs for capacity to identify pathogen specific infections shows just how lowly we score on that. At best, the average is just two such labs at each of the district level save for big cities and towns which may have more. Self-medication is the other likely culprit particularly vogue in Kenya. In many set-ups purchase of antibiotics over the counter is the norm. Urinary Tract Infections and Respiratory Tract Medications are especially routinely purchased over the counter. No wonder these are some of the most affected drugs. The non-adherence issue is at the health worker’s reach and should be addressed through concerted and sustained education of health workers and the public on the dangers of such behavior. What medics cannot do is to ensure the quality and strength of the antibiotics in the market is as required; this is the job of the pharmacovigilance department and they should ensure that regular and sustained evaluation of potency of drugs is done. Regular checks for developing resistance patterns should also be scaled up by epidemiologists to identify resistance patterns early. As scheduled drugs, Pharmacists should ensure that antibiotics are only dispensed when need exists and not just for the sake of making a sale.Drug manufacturers and marketers too need to join the fight to support safer and more responsible use of their products by fighting counterfeits. This article is adopted from the Business Daily Health and Life section section as writer by Edward Omete Back to top |
| Kenya's New Healthcare Nightmare |
 |
|
Pneumonia is a common acute respiratory infection that attributes to a high mortality rate in the world. In the recent past Malaria has been the top killer disease in Kenya however, that is now a thing of the past. Official data shows pneumonia killed 22,473 Kenyans last year upto 21,640 the previous year, while casualties from malaria which for years has been the top killer declined by 22,267 to 20,691.Most of those affected were children under five. Kenya was among the first countries in the East African Region to introduce PCV, and the first low-income country to use then ten-valent vaccine. Today, new-borns nationwide receive the vaccine in 3 doses at 6, 10 and 14 weeks. Kenya’s push to immunize babies against pneumonia has helped the country advance on the 2025 targets of the Integrated Global Action Plan for the Prevention and Control of Pneumonia and Diarrhoea (GAPPD), released by WHO and UNICEF in 2013. Pneumococcal vaccine, a key element of the new integrated strategy had been introduced in 102 countries by the end of 2013, and global coverage was estimated at 25%. Since PCV-10 was introduced in Kenya, scientists at the Kenya Medical Research Institute (KEMRI) have been studying the impact of the vaccine on children's health. Their research which is supported by the Wellcome Trust and Gavi found that the introduction of PCV-10 in Kenya resulted in an estimated 42.7% reduction in pneumococcal disease episodes and a 6.1% reduction in childhood deaths. The question arising is why the sudden rise in pneumonia related mortality despite such ardent measures to fight this dilemma? According to Health Principle Secretary Nicholas Muraguri, indoor smoking as well as the use of kerosene and wood fuel for lighting and cooking especially in rural Kenya was behind the surge in Pneumonia deaths. In the past year Pneumonia did not receive so much attention like TB, Malaria and HIV/Aids which happened to benefit greatly from increased publicity as well as free treatment across the country. It could be then argued that neglect is the cause behind the sudden shift in statistics In the fight against these life threatening diseases in Sub-saharan Africa the Government should perhaps formulate a strategy that equalizes the efforts shoved towards the fight against key killer diseases by facilitating adequate publicity and education to the general public and ultimately provide easy, efficient and effective accessibility to treatment as well Make a once time life opportunity and volunteer abroad during your gap year and help Africa in its fight against Pneumonia and Malaria which is killing hundreds of children yearly. Back to top |
| A Dual Survivor of Epilepsy and Bipolar Condition |
 |
|
Sitawa Wafula is a Mental Health Activist and a Social Media enthusiast. A multi-talented Artist and a Poet who advocates through all forms of media for more attention and awareness in Mental Health. She decided to share her personal struggle with Bipolar condition by starting her free Mental Health text line project to reach out to patients and affected families. At least one in every four people (11.5 million Kenyans) will suffer from some form Mental illness at one point in their lives, health experts warned during the launch of the Mental Health Policy 2015-2030. Mental Health is described as a state of well-being where individuals recognize their abilities, are able to cope with normal stresses of life, and work productively to make a contribution to their communities. According to the Africa Research Institute (AFI), Public health researchers often group Mental illnesses into five categories: 1) common mental disorders (including depression and anxiety), 2) severe mental disorders (including psychosis, schizophrenia and bipolar disorder), 3) neurological disorders (such as epilepsy and dementia), 4) childhood disorders and 5) substance and alcohol disorders. One interesting disparity with Europe and North America is that epilepsy is categorized as a mental disorder in Kenya and in other parts of Africa as opposed to the other regions. The Integration of mental health into primary care in Kenya, article in World Psychiatry, 2010 says that the Mental Health care in Kenya is predominantly Government funded, but remains extremely limited in terms of infrastructure, manpower and finances. Mental health specialist care is largely delivered at county level hospitals by psychiatric nurses running outpatient clinics and by the national referral hospitals at Mathari Mental Hospital, University of Nairobi and at the Moi University Teaching and Referral Hospital (MTRH) the total number of mental health hospital beds for the for a 40 million people was 1114 in 2009. Thus the specialist service for nearly all regions and counties is largely delivered by extremely overstretched mental health nurses, who have had hardly any access to continuing professional development throughout their careers. Sitawa discovered after a traumatic experience a Bipolar Disorder Diagnosis and Epilepsy discovery that there was not much information around that she could access to help her understand how to cope and further understand her physical and mental health. Consequently, there was a lot of social stigma surrounding her mental health which made the process of dealing with things even more challenging, she notes on her blog profile. In her commitment to advocating for better Mental Health care services, Sitawa started a Mental Health social enterprise called My Mind My Funk (MMMF) along with Kenya’s first free mental health SMS help line 22214, which has helped survivors of rape and people living with epilepsy and mental disorders all over Kenya, different parts of Africa and the world. MMMF is focused on the social and preventative aspects of mental health as opposed to the curative which in too many cases involves traditional healers or subpar psychiatric help. The organization tries to include Mental Health Awareness in everyday life by working with young people to promote wellness in their communities all across Africa. This way according to her, “you don’t need to always contact Sitawa or MMMF to get information on mental health,” and you can access mental health information that is suited to you. She uses her personal journey as a rape survivor living with a dual diagnosis of epilepsy and bipolar to provide people in Africa with the necessary information and support to not only handle mental health conditions but also deal with everyday life. She achieves this through her Google Award winning self-titled blog (http://sitawa.blogspot.co.ke) and her mental health social enterprise; My Mind, My Funk which ran Kenya’s first free mental health support line and provided support to over 11,000 Kenyans. Her remarkable work to bring conversations that are tabooed in Africa on the table saw Sitawa appointed the Mental Health Youth Ambassador because she was very vocal about her bipolar condition in 2010. She was crowned the 2013 Activist of the Year and East Africa Youth Philanthropist. She was named as a Non Communicable Disease Champion by the Ministry of Health – Kenya and recognized among the top 40 under 40 women in Kenya, 2015 and her work featured in various national and international media outlets including BBC and Al-Jazeera. The prestigious Aspen Institute recently named her among the New Voices in their 2016 list of emerging experts from developing countries. Sitawa’s campaigns aimed at amplifying the voices of people living with mental health conditions in Africa saw the Ministry of Health – Kenya launch and adopt the Mental Health Policy 2015-2030. Which the ministry now says, (policy) will not only streamline the laws guiding the neglected area but also help in drafting more laws to govern the practice and care offered to patients. "We have not been operating in a vacuum but the policy was necessary to guide how laws are enacted as well as identifying gaps in the sector," the Health Cabinet Secretary Dr Cleopa Mailu explained. He added: "With this policy, we intend to attain high standards of care for these patients."Through creating awareness and advocating for better health care system, Sitawa has changed how many people in Kenya and Africa view and think about mental health. Advocacy is a key tool in attainment of health goals because it is the empowerment of people to speak out and seek solutions to the health issues that confront them on a daily basis. Elective Africa organizes psychiatric internships at Port Reitz Hospital in Mombasa where our students receive hands on experience which is very important as they advance their career in this area. If you are interested contact us for more information. Back to top |
|
|

 6 2016
6 2016